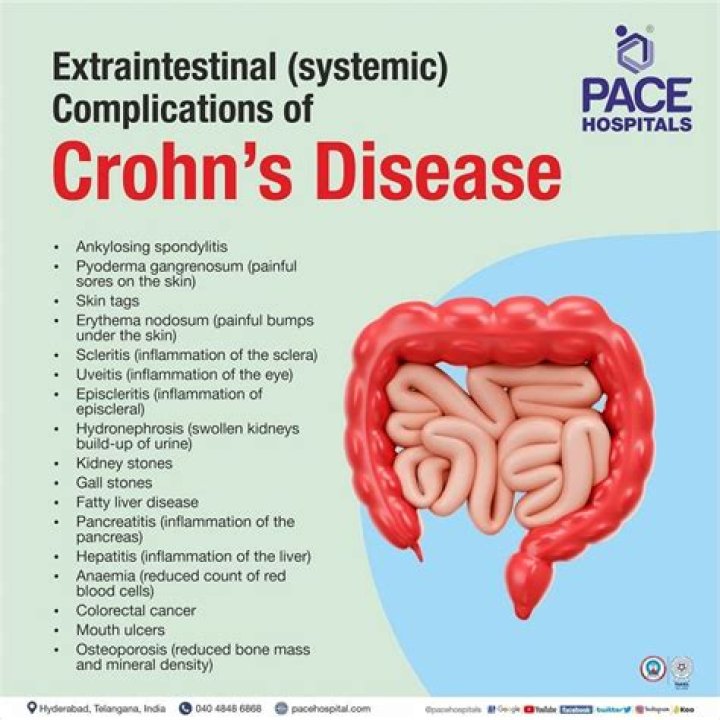
Enteropathic arthropathy or enteropathic arthritis refers to acute or subacute arthritis in association with, or as a reaction to, an enteric (usually colonic) inflammatory condition..
Also asked, what are the symptoms of Enteropathic arthritis?
Classic enteropathic arthritis symptoms include:
- Back pain or stiffness. Enteropathic arthritis may cause back pain or stiffness, especially in the mornings, but the discomfort usually gets better as you move throughout the day.
- Swollen, red, painful joints.
Beside above, how is Enteropathic arthritis treated? Treatments
- Non-Steroidal Anti-Inflammatory Drugs for Inflammation and Pain. Non-Steroidal Anti-Inflammatory Drugs can reduce the inflammation caused by Enteropathic Arthritis and can help reduce pain symptoms.
- Disease Modifying Anti-Rheumatic Drugs.
- Biologics.
Similarly, you may ask, what causes Enteropathic arthritis?
Enteropathic arthritis is an inflammatory condition affecting the spine and other joints that commonly occurs in the inflammatory bowel diseases – Crohn's disease and ulcerative colitis. Other spondyloarthropathies include ankylosing spondylitis, psoriatic arthritis, and reactive arthritis.
How do you know what type of arthritis you have?
Your doctor can't use any single test to determine if you have RA. To develop a diagnosis, they'll likely take a medical history, conduct a physical exam, and order X-rays or other imaging tests. Your doctor may also order a: rheumatoid factor test.
Related Question Answers
Can you be fat and have Crohn's disease?
Background and aims: Obesity and overweight are major public health issues. Although traditionally associated with weight loss, there is now evidence that increasing Body Mass Index (BMI) and overweight are emerging features of Crohn's disease (CD) and may be associated with more severe disease course.What does Crohn's arthritis feel like?
Symptoms include pain and stiffness in your lower spine and near the bottom of your back at the sacroiliac joints. Some people may even have symptoms of AS months or years before their Crohn's disease symptoms appear. This type of arthritis can lead to permanent damage.Can you get arthritis from Crohn's disease?
It may affect as many as 30% of people with Crohn's disease or ulcerative colitis. Although arthritis is typically associated with advancing age, in IBD it often strikes younger patients as well. In addition to joint pain, arthritis also causes swelling of the joints and a reduction in flexibility.Are ulcerative colitis and rheumatoid arthritis related?
Ulcerative colitis (UC) is a colonic disease characterized by chronic inflammation. Rheumatoid arthritis (RA) is a rheumatological chronic inflammatory disease characterized by joint swelling and tenderness. It is also considered an autoimmune disorder. Arthritis is the most common complication of ulcerative UC.Is ulcerative colitis linked to arthritis?
Two types of conditions can affect the joints in people with ulcerative colitis. Arthritis in people with ulcerative colitis doesn't usually cause long-term joint damage. The joints swell up and become painful, but they return to normal once intestinal inflammation is under control.Can osteoarthritis cause digestive problems?
But research shows tummy troubles are common among people with inflammatory arthritis: A study published in the Journal of Rheumatology found that rheumatoid arthritis patients have a 70 percent greater chance of developing a gastrointestinal (GI) problem compared to people who don't have RA.What is Enteropathic arthropathy?
Enteropathic arthropathy is an umbrella term used to describe various patterns of inflammatory arthritis which may be associated with a range of gastrointestinal (GI) pathologies. Its constituent conditions are classified as part of the seronegative spondyloarthropathies.What is septic arthritis?
Septic arthritis, also known as joint infection or infectious arthritis, is the invasion of a joint by an infectious agent resulting in joint inflammation. Most commonly, joints become infected via the blood but may also become infected via trauma or an infection around the joint.What is Whipple?
Whipple disease is a rare bacterial infection that most often affects your joints and digestive system. Whipple disease interferes with normal digestion by impairing the breakdown of foods, such as fats and carbohydrates, and hampering your body's ability to absorb nutrients.Can Crohn's disease cause joint pain?
Joint pain can be a common symptom of Crohn's disease. As many as 30 percent of people with an inflammatory bowel disease (IBD), such as Crohn's or ulcerative colitis, experience arthritis — inflammation and pain in the joints — at some point in their lives, according to the Crohn's and Colitis Foundation.Is there a link between Crohn's disease and rheumatoid arthritis?
Explaining the Link Between Crohn's and Arthritis Some recent research suggests an overlap between Crohn's disease and other autoimmune arthritis conditions, such as psoriatic and rheumatoid arthritis. Both Crohn's and rheumatoid arthritis are categorized as immune-mediated inflammatory diseases.Can Crohns disease cause hip pain?
This case is unusual in that complications from Crohn's disease rarely present as hip pain, but rather as abdominal complaints. Also, iliopsoas bursitis is a rare but known cause of hip pain, it usually is associated with hip joint pathology, such as degenerative or inflammatory conditions like rheumatoid arthritis.What is the best treatment for spondylitis?
Medications. Nonsteroidal anti-inflammatory drugs (NSAIDs) — such as naproxen (Naprosyn) and indomethacin (Indocin) — are the medications doctors most commonly use to treat ankylosing spondylitis. They can relieve your inflammation, pain and stiffness.Does IBS cause arthritis?
People with IBS may be more likely to experience joint pain. Scientists still do not know why, but it may be due to increased inflammation in the body. A 2017 study found that people with IBS had an increased risk of a type of joint pain called temporomandibular disorder.What type of arthritis is associated with Crohn's disease?
Enteropathic arthritis, or EnA, is a form of chronic, inflammatory arthritis associated with the occurrence of an inflammatory bowel disease (IBD), the two best-known types of which are ulcerative colitis and Crohn's disease.Can digestive problems cause joint pain?
Share on Pinterest Joint pain is a potential symptom of ulcerative colitis. While most of the common symptoms of UC are gastrointestinal, such as bloating, diarrhea, and bloody stool, this disease can also affect other parts of the body. Arthritis, a term that covers joint pain, inflammation, swelling, and redness.Can chlamydia cause arthritis?
Reactive arthritis is a type of arthritis caused by an infection. It may be caused by Chlamydia trachomatis, salmonella, or another infection. The condition may cause arthritis symptoms, such as joint pain and inflammation. It may also cause symptoms in the urinary tract and eyes.Does leaky gut cause arthritis?
Leaky gut syndrome and other gastrointestinal problems could trigger flare-ups in diseases like RA, lupus, and multiple sclerosis. In fact, the gut microbiome has been linked to arthritis in various animal studies.Can microscopic colitis cause joint pain?
Doctor's response. The primary symptom of microscopic colitis is chronic, watery diarrhea . Patients with microscopic colitis can have diarrhea for months or years before the diagnosis is made. Patients with autoimmune disorders can develop joint pain and stiffness.